An individual’s risk of falling is multifactorial, shaped by muscle strength, balance, mobility, and overall physical resilience.
Able Assess applies this understanding through a multifactorial, evidence-based approach, providing clinicians and care professionals with a fast, standardized, and clinically validated tool for identifying at-risk individuals.
By combining four objective, validated measures – Grip Strength, the 30-Second Chair Stand Test (CST), the Timed Up and Go (TUG) test, and the 4-Meter Gait Speed (4MGS) test – Able Assess delivers a comprehensive falls risk profile in under five minutes. This approach enables early risk identification, enhances older adult safety, and provides actionable, data-driven insights to guide downstream interventions.
Chair Stand Test (CST): Lower Limb Strength and Endurance
Lower limb strength is essential for mobility, balance, and maintaining independence. The 30-Second Chair Stand Test (CST) is a validated, practical measure of lower-body strength and endurance that directly reflects an individual’s ability to perform daily activities.
Regular CST assessment helps identify individuals at risk of functional decline, enabling timely interventions that preserve strength and autonomy (Kulkarni et al., 2023; Buatois et al., 2008).
Evidence Base: Chair Stand Test
- Recommended by the CDC’s Stopping Elderly Accidents, Deaths & Injuries (STEADI) initiative for lower limb strength assessment.
- Recognized by the World Guidelines for Falls Prevention (WGFP) as a key screening measure for reduced muscle strength, alongside grip strength.
Clinical Thresholds and Interpretation (Able Assess)
Able Assess applies the CDC STEADI’s age- and sex-specific thresholds, derived from a U.S. cohort of 7,183 community-dwelling older adults across 21 states. Results are categorized as Below Average, Average, or Above Average based on these standards, as shown in the tables below:
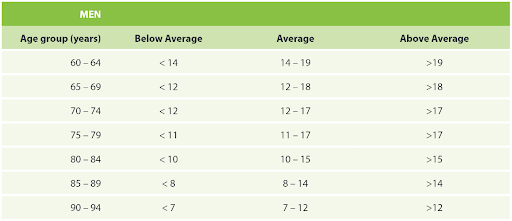
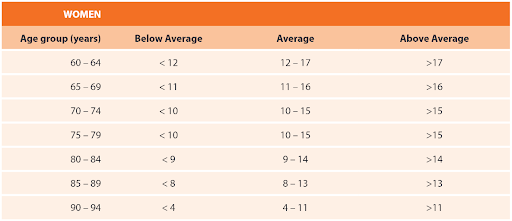
(Note: In accordance with CDC recommendations, risk scores are calculated for adults ≥60 years.)
Clinical Relevance: Chair Stand Test
By aligning with the CDC’s validated CST thresholds, Able Assess provides clinicians with a reliable, standardized measure of lower limb strength – a critical determinant of mobility and fall risk.
Timed Up and Go (TUG): Dynamic Balance and Functional Mobility
The Timed Up and Go (TUG) test is one of the most widely validated assessments of dynamic balance, gait, and mobility. It is recommended by multiple clinical guidelines, including the CDC STEADI toolkit, the American and British Geriatrics Societies, and the UK’s National Institute for Health and Care Excellence (NICE) guidelines.
Evidence Base: Timed Up and Go
- Published cut-offs range from 13–32.6 seconds, reflecting variation in populations and methodologies.
- The CDC STEADI recommends a 12-second threshold to identify elevated falls risk.
- A recent study showed that this same 12-second cut-off also predicts hospitalization-associated functional decline (HAFD) in older adults.
Clinical Thresholds and Interpretation (Able Assess)
- <12 seconds (green) = Normal
- ≥12 seconds (orange) = Below Normal
(Note: Risk scores are applied for adults ≥65 years, consistent with CDC guidance.)
Clinical Relevance: Timed Up and Go
A single cut-off improves consistency and interpretability in clinical practice. The CDC’s 12-second threshold is widely accepted as a sensitive, practical benchmark for identifying individuals who may require further assessment or intervention.
4-Meter Gait Speed (4MGS): Mobility and Functional Reserve
Gait speed is an established “vital sign” of aging – a simple yet powerful predictor of mobility, health status, and survival. The 4-Meter Gait Speed (4MGS) test provides a reproducible, quantitative measure of walking velocity that correlates strongly with independence and resilience.
Evidence Base: 4-Meter Gait Speed
- Recommended by the WGFP and multiple international guidelines as a core component of falls and functional decline assessments.
- Standard thresholds vary by population:
- ≥1.0 m/s – Normal for community-dwelling older adults without disability
- <0.8 m/s – Indicative of increased falls risk in lower-functioning adults
- ≥1.0 m/s – Normal for community-dwelling older adults without disability
Clinical Thresholds and Interpretation (Able Assess)
Able Assess follows WGFP guidelines:
- 0.8 m/s (green) = Normal
- ≤0.8 m/s (orange) = Below Normal
(Note: Risk scores are applied for adults ≥65 years.)
Clinical Relevance: 4-Meter Gait Speed
Because gait speed reflects overall physical capacity and functional reserve, tracking it over time provides a sensitive indicator of both decline and improvement. Its inclusion within Able Assess enables reproducible monitoring of mobility and independence.
Grip Strength: Indicator of Overall Health and Frailty
Grip strength is one of the most widely validated biomarkers of physical function and resilience. It provides a quick, non-invasive measure of global muscle strength and physiological reserve.
Evidence Base: Grip Strength
- One of five criteria defining frailty within the Fried Frailty Phenotype (FFP).
- A diagnostic marker for sarcopenia according to the European Working Group on Sarcopenia in Older People (EWGSOP2).
- Cohort studies link weak grip strength to increased falls risk, particularly in older women with impaired balance.
- Several studies confirm that weak grip strength correlates with impaired mobility, and increased risk of disability.
Clinical Thresholds and Interpretation (Able Assess)
Able Assess benchmarks grip strength against a live, continuously updated normative dataset built from UK and U.S. digital measurements. This percentile-based model allows for accurate population comparisons and longitudinal tracking of decline.
Clinical Relevance: Grip Strength
Grip strength offers clinicians a fast, objective indicator of systemic resilience and frailty. When integrated with other physical function measures, it enhances the precision of falls risk profiling and supports targeted interventions.
The Power of a Multifactorial Approach
Falls are inherently multifactorial – no single test can capture the complete picture of an individual’s risk, as emphasized by recent international NICE guidelines on falls prevention. Able Assess was designed to bridge this gap by combining CST, TUG, 4MGS, and Grip strength into a single, standardized assessment platform.
Synergistic Assessment
- CST highlights lower-limb weakness
- TUG reflects mobility and balance
- 4MGS captures global functional reserve
- Grip strength reflects systemic resilience
Together, these measures form a holistic physical function profile.
Enhanced Predictive Validity
Studies show that combining multiple functional assessments improves predictive accuracy for adverse outcomes compared to single tests alone. Able Assess’s multifactorial design strengthens risk stratification and supports data-driven clinical decision-making.
Targeted, Personalized Interventions
This combined dataset allows clinicians to match evidence-based interventions to each patient’s needs, such as resistance training for low CST or grip performance, balance training for impaired TUG, or multidisciplinary support for slow gait speed.
Conclusion
In under five minutes, Able Assess delivers a standardized, clinically grounded, and multifactorial falls risk profile aligned with both U.S. and international best practice.
Its integration of strength, mobility, and balance measures ensures clinicians can identify at-risk individuals early, monitor progress over time, and intervene effectively to reduce falls and preserve independence.
Read more from Able Care
In our next article, we explain what to expect at an Able Assess fall risk screening.
Find out more about falls prevention in our dedicated articles.
For further reading, explore our extensive collection of studies on using a hand dynamometer, grip strength and more including:
- Grip Strength and Longevity
- Grip Strength for Frailty
- Grip Strength and Surgery
- Grip Strength and Respiratory Disease
- Grip Strength and Oncology
- Grip Strength and Renal Disease
- Grip Strength for Gastrointestinal Disease
- Grip Strength and Heart Disease
- Grip Strength and Metabolic Diseases
- Grip Strength and Sport: Grip Strength as a Biomarker for Sports Performance
- Grip Strength in Sports Medicine: Use Cases and Recommendations
- What are Biomarkers? The Role of Grip Strength in Modern Healthcare
- The Importance of Functional Health Measurements
- The Role of Grip Strength Measurements for GLP-1 Administration
- Hand Dynamometer Guide
- Able Assess User Guide
Our market-leading technology and data platforms drive early detection of functional health issues such as falls risks, track outcomes and support true value-based healthcare.
Contact us at hello@able-care.co for more information. We have best-in-class products for every stage of your functional health journey. To see our technology in action, book a demo.

